Fetal Diagnostics
Introduction
At the Zurich Center for Fetal Diagnosis and Therapy we cover the entire range of diagnostic services available in the world today. In the event that an investigation cannot be performed in Zurich, samples can be sent anywhere in the world for analysis, ensuring you receive the best possible care.
First trimester screening
First trimester screening can tell whether a child will be affected by a chromosome abnormality, most commonly trisomy 21, 13, or 18.
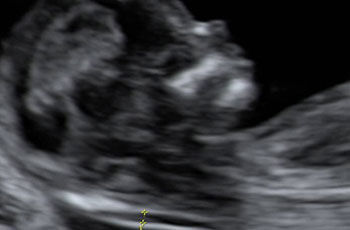
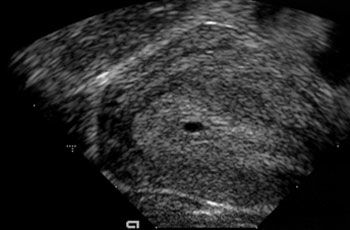
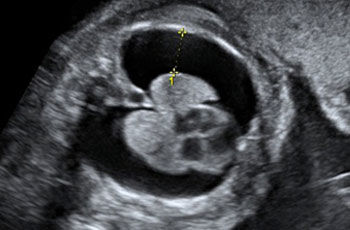
Along with a blood test, measurement of nuchal (nape of the neck) translucency thickness (1) forms an essential part of first trimester screening.
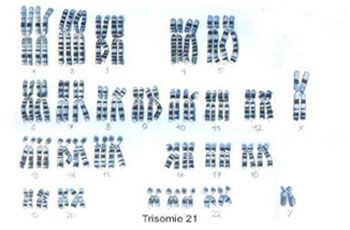
Experience shows a correlation between increased thickness of the nape of the fetal neck and the probability of trisomy 21 (2).
Ultrasound scanning
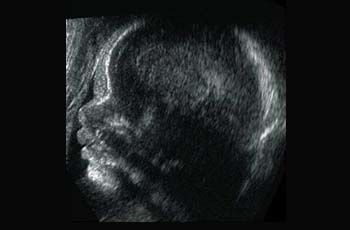
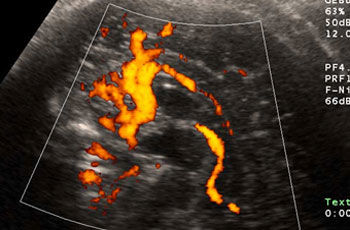
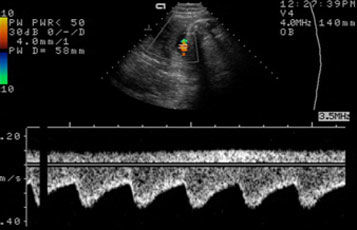
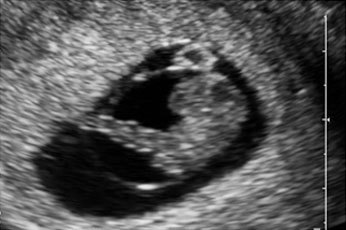
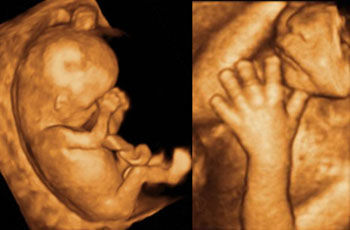
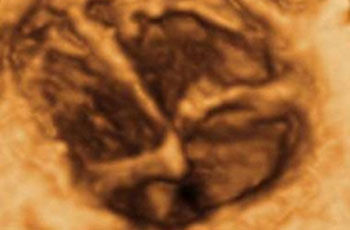
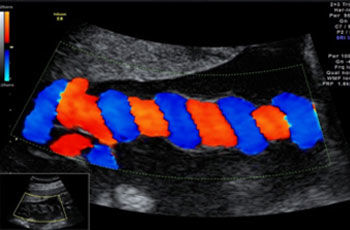
An ultrasound scan can show the presence of an amniotic sac in the uterus immediately after the first missed period (1). After only six weeks the embryonic heart is beating and the embryo can be visualized (2). A check is performed later to confirm that only one embryo is present and to determine whether the embryo is developing normally and all its organs are correctly formed. In the second half of pregnancy the fetus has a recognizable face (3). Special techniques visualize the fetal blood vessels, e.g. in the brain (4). Other techniques can measure the direction and velocity of blood flow and thus provide information on the perfusion of various organs (5). Using 3D ultrasound even a lay person can easily recognize the developing fetus (image of fetus at week 11 of pregnancy). Details such as the hands and face can be seen very vividly (6).
Echocardiogram
An echocardiogram is an ultrasound scan of the heart. The heart is by far the most difficult fetal organ to image. 3D ultrasound is useful for identifying the ventricles and atria.
Fetal MRI
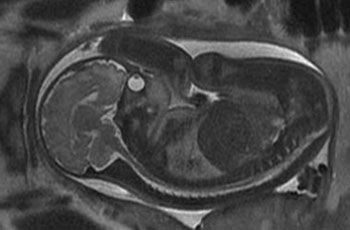
In some cases diagnostic ultrasound scans are complemented by magnetic resonance imaging (MRI) of the developing child. MRI is always valuable when ultrasound comes up against its limits, e.g. in maternal overweight, absence of amniotic fluid, or unfavorable fetal lie. The fetal brain can be visualized particularly well. Unlike with ultrasound, the whole child is always imaged. The images become somewhat blurred if the mother or child makes any brisk movement. Like ultrasound, MRI is completely harmless to the fetus.
Amniocentesis
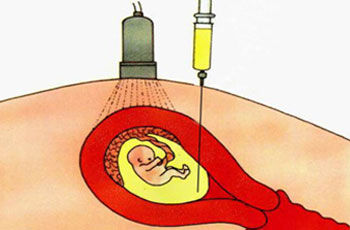
In amniocentesis a fine needle is inserted into the uterus under ultrasound guidance and a sample of amniotic fluid is taken. The fetal cells floating in the amniotic fluid can be used for genetic analysis. As amniotic fluid consists mostly of fetal urine, the fluid that is removed is rapidly replenished.
Chorionic villus sampling (biopsy of the fetal placenta)
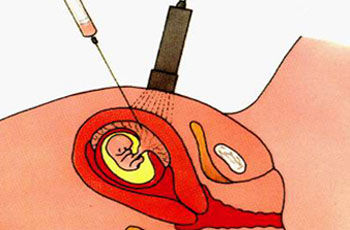
In chorionic villus sampling a fine needle is inserted under ultrasound guidance into the chorion, which later gives rise to the fetal placenta, and small tissue fragments are aspirated into a syringe. These tissue samples are used for genetic analysis.
Fetal thoracentesis
Sometimes, e.g. because of a malformation, fluid accumulates around the fetal lungs (black region between the yellow marks in the illustration). This fluid can be aspirated through a fine needle to determine the cause.
Umbilical vein sampling (cordocentesis)
Sometimes a fetal blood sample is needed to investigate certain diseases. Great skill is required to cannulate the thin umbilical vein (shown as blue in the illustration).
Genetic testing
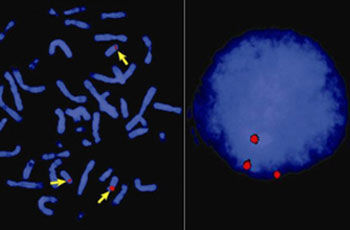
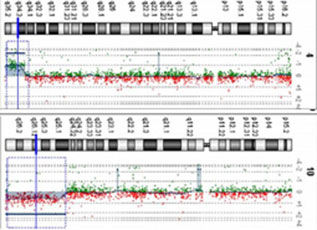
Chromosomes of dividing cells are firstly stained. The resulting pattern of bands, similar to a barcode, is specific for a particular chromosome (1). The geneticist checks to see whether exactly two copies of the chromosome are present in each cell and whether the pattern of bands shows a correct sequence. In urgent cases chromosomes can be visualized by using dyes (2). This can be done both in dividing cells (image on the left) and in cells that are not dividing (image on the right). In both cases the cells of this fetus show three colored dots, suggesting the presence of trisomy. Comparative genomic hybridization (CGH) is a newly developed method that we use in selected cases where we suspect a genetic illness (3).